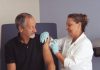
Compared to the expected deaths plus COVID-19 deaths, estimates of all-cause mortality during the SARS-CoV-2 pandemic were markedly higher.
The Coronavirus disease 2019 (COVID-19) has caused immense suffering to the global human community. As of January 28, 2021, the virus has infected more than 100 million people and killed 2,199,406 people worldwide.
With the progression of the pandemic, there has been a growing focus on the number of deaths related to the disease. Many believed that the actual number of deaths, particularly in Europe and the USA, would be much lower than what we see on the media.
However, emerging data from multiple studies tell us different stories. Compared to the expected deaths plus COVID-19 deaths, estimates of all-cause mortality during the pandemic were markedly higher. It means excess mortality during the pandemic emerged from both COVID and non-COVID deaths.
Excess mortality from COVID-19 appears in several studies that also investigated total mortality during the pandemic.
In Germany, for example, during the weeks 10 to 23 in 2020, the estimated excess number of deaths was 8071 (8674 deaths according to Robert Koch-Institute) (Stang, Standl et al. 2020).
In England, from April 10 to May 8, the deaths of recipients of domiciliary care were 2.7 times the three-year average for that period. From April 10 to May 1 (the latest available data), deaths of care home residents were 2.8 times or 3.2 times that of the same period in 2019 (Glynn, Fielding et al. 2020).
In Italy, 38921 excess deaths were recorded in three macro-region areas, like North West, Lombardia, and North East areas, with over 86% of the expected total deaths from February 22 to April 28, 2020 (Blangiardo, Cameletti et al. 2020).
Excess mortality in 24 EuroMOMO countries, including the UK, showed an increasing trend during the first weeks of March 2020. The cumulative excess mortality from week 1 to week 18, 2020, reached 185,287 deaths (Vestergaard, Nielsen et al. 2020).
In Brazil, from March to May 2020, 39,146 excess deaths were recorded, and the rate was higher among men (Silva, Jardim, et al. 2020).
A study led by researchers at Virginia Commonwealth University shows that deaths between March 1 and August 1 in the USA increased by 20% compared to previous years 2014 to 2019 (Woolf, Chapman et al. 2020a).
A similar report by the same authors from VCU and Yale University focused on data from March to May 1 also found 87,001 excess death, which is a 20.2% increase compared to the previous years (Woolf, Chapman et al. 2020b).
While reporting excess mortality directly by COVID-19, several studies have also estimated the number of deaths caused by the pandemic indirectly.
For example, in the Virginia study, researchers have shown that only 67% of those excess deaths were attributed to COVID-19, and the remaining one-third were due to other causes, such as dementia and heart disease (Woolf, Chapman et al. 2020a).
In the UK, as of May 1, 2020, 28% of excess deaths did not involve COVID-19. Spain, which has seen the highest excess mortality per million population in the EU, a significant proportion, 39% of excess mortality, was not directly related to COVID-19.
From March 1 to July 31, 2020, a total of 76,088 all-cause deaths occurred among US adults aged 25 to 44years, which was 11,899 more than the expected 64,189 deaths. However, only 38% of all-cause excess deaths recorded during the pandemic were attributed directly to COVID-19 (Faust, Krumholz, et al. 2020).
Older age, sepsis, hypertension, diabetes, prolonged use of non-invasive ventilation, weakening immune system, and abnormal blood clotting were among the major causes of direct COVID-19 fatalities. Poorer outcomes of the patients might be partially responsible for increased inflammation causing damage to the heart, brain, and other vital organs.
Other factors that increased the mortality during the pandemic indirectly include personal risk factors that were not properly taken care of, attitude toward restrictions measures, public health policies, emotional crises, and fears of contracting the disease.
For example, in the USA, the number of patients reporting heart attacks and strokes has declined during the pandemic (Kansagra, Goyal, et al. 2020). Urgent referrals for suspected cancer have fallen in many countries. While prioritizing COVID-19 cases, standard care for other cases may have been obstructed.
Globally, the World Health Organization has found that more than half (53%) of the countries have partially or entirely disrupted services for hypertension treatment; 49% for treatment for diabetes and diabetes-related complications; 42% of countries have experienced disruption for cancer treatment, and 31% for cardiovascular emergencies (WHO 2020).
Many believe that if COVID-deaths is reduced at the cost of life from other causes, the efficacy of the pandemic response will be in question. Therefore, assessing the pandemic’s secondary health impacts—from restricted drug use and domestic violence to reduced access to standard medical care—which could contribute to loss of life, is urgent.